Don’t Dismiss Brain Imaging as an Academic Gimmick
In a pair of views from our partner site The Conversation, two exponents of brain research discuss the utility of brain imaging technology. Here, Matt Wall takes a more optimistic view, while in the companion post, Catherine Loveday takes the less enthusiastic view.
***
Given the media coverage brain imaging studies get, you might think that they are constantly revealing important secrets about this mysterious organ.
Catherine Loveday thinks otherwise. She makes the point that using brain-scanning technology to understand what a diseased brain is doing is only of academic interest. It is the study of the mind through behavior and other cognitive functions, she argues, that leads to useful insights about disorders and treatments.

This piece by Matt Wall originally appeared at The Conversation, a Social Science Space partner site, under the title “You can’t dismiss brain imaging as just an academic gimmick.”
There is some truth here, but as a scientist who uses brain scans every day, I would argue that they contribute a lot more than Loveday gives them credit for.
The main problem is that, when it comes to the brain, all analogies are hopelessly crude. The distinction between hardware and software – or the brain and the mind – only has limited practical usefulness. Since all mental processes arise as a result of brain processes, it follows that all mental problems are also a result of dysfunctions in the physical brain.
This will be seen by many as an extreme and reductionist position, but a specific example should help to show that it has some value.
Parkinson’s disease is a degenerative disorder that causes a variety of symptoms including motor problems, sleep disturbance, various cognitive issues, and often depression. This variety of symptoms might suggest that the underlying problem in Parkinson’s is quite broad and complex, affecting several brain systems. However, it turns out the cause of all these symptoms is quite specific: a loss of neurons in a region of the brain called the substantia nigra.
The wide variety of symptoms in Parkinson’s is produced by projections from this region that influence other brain areas. Parkinson’s then, is a clear hardware problem, and is in fact amenable to hardware-based treatments. Many patients have now been implanted with deep-brain stimulation devices which electrically stimulate neurons in the problem area to increase their activity. Such devices can be remarkably effective in controlling the symptoms of Parkinson’s.
Our current understanding of Parkinson’s disease owes a large debt to brain scanning research. The TransEuro project is a current research program involving 15 institutions across Europe to investigate the use of stem-cell treatments in Parkinson’s. Positron emission tomography (PET) and magnetic resonance imaging (MRI) form a cornerstone of the research in this project, as well as in many others. Brain scans are also often used clinically to rule out alternative diagnoses in cases of suspected Parkinson’s.
Another startling example comes from the work of Adrian Owen, of the University of Waterloo, on patients in a persistent vegetative state. These are people who have suffered serious injuries or diseases leading to being unresponsive to any external stimuli. They can’t move, talk, or respond in any way.
Until recently, it was unknown whether these patients were truly unconscious, or whether they had some awareness of their surroundings and just could not respond. Starting in 2006, Owen and his colleagues have shown that some of these patients are able to respond meaningfully, proving that they are indeed aware of their environment. They achieved this by using functional brain scans to measure brain activity in patients as questions were asked. One patient has even learned to change his brain activity in such a way that he is able to answer “yes” or “no” to questions.
The main problem is that, when it comes to the brain, all analogies are hopelessly crude. The distinction between hardware and software – or the brain and the mind – only has limited practical usefulness
In these cases there is no way to access the patients’ mind through studying their behavior or asking them questions. Accessing their brain activity through functional scans is the only communication option left. The demonstration that some of these patients are in fact conscious has important implications for patient care, medical ethics, and clinical decision-making.
Most other mental problems are unfortunately not nearly so clear-cut as Parkinson’s, or (fortunately) so extreme as a vegetative state. Describing the underlying brain problem in, say, autism, depression, or schizophrenia is more difficult, and our understanding of these disorders is therefore less advanced. It seems likely that these issues are probably associated with more subtle problems, across several brain regions. Some may even be undetectable with current technology, however that is a practical issue and will hopefully be resolved as the technology improves. Just because we can’t currently visualize all the brain effects associated with these disorders doesn’t mean they don’t exist.
The most fruitful approach when trying to gain understanding about something as complex as mental disorders is to use all the sources of evidence available. That means integrating results from brain imaging, animal models, genetics, and studies of behavior and cognition too.
No matter how impressive brain-scanning technology becomes, there will always be a need for people who understand cognition and behavior to design the right experiments that will produce the most valuable and useful results from the technology. Using the two approaches together creates a powerful set of tools that can potentially produce practical, clinically helpful information, as well as amazing scientific results.![]()
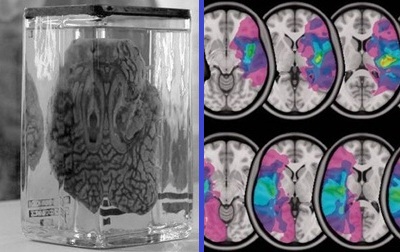
































































































“Until recently, it was unknown whether these patients were truly unconscious, or whether they had some awareness of their surroundings and just could not respond. Starting in 2006, Owen and his colleagues have shown that some of these patients are able to respond meaningfully, proving that they are indeed aware of their environment. They achieved this by using functional brain scans to measure brain activity in patients as questions were asked. One patient has even learned to change his brain activity in such a way that he is able to answer “yes” or “no” to questions.” It is not too… Read more »