The Need for a Social Identity Analysis of COVID-19: Introduction to ‘Together Apart’
As we write, at the start of May 2020, 4 million people have been infected with the COVID-19, over a quarter of a million have died and more than a third of the entire population of the planet is under some form of restriction of movement. It is the biggest health emergency of our generation. And yet, unless or until a vaccine is developed, or we discover medicines to treat the virus, our means of controlling the spread of infection depend on behavioural changes and hence upon human psychology.
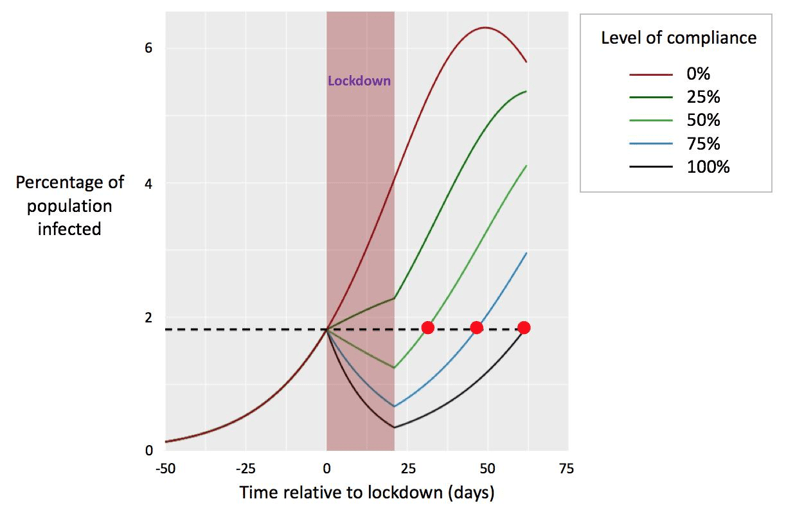
This is most obvious in the case of lockdown. While it is all very well to tell people that they must stay at home in order to flatten the curve of infection, the effectiveness of the policy depends on whether or not they do. Just how sensitive the curve is to even minor changes in compliance is made clear by Figure 1, which was created at the end of March by Mark Woolhouse — one of the epidemiologists advising the UK government. As this graph shows, a fully compliant population could reduce the proportion of those infected at the end of a 3-week lockdown by a factor of 10: from 4.1% to under 0.4%. In Britain, this would amount to a vast difference in infection numbers — from approximately 2.75 million to 270,000 people infected. Similar calculations around the world have inspired many government-led campaigns to encourage people to ‘Stay at Home and Save Lives’. Behaviour, then, is clearly critical. Indeed, all we can do to control the virus right now is get people to behave appropriately — to ‘do the right thing’.
A sceptic might retort that this is a matter of picking low-hanging fruit. Of course, the lockdown is a matter of changing what people do. But one of its key aims is to give us time to prepare and reduce the levels of infection so that they can then be dealt with by other types of intervention. This sceptic’s argument suggests that as the days of lockdown are numbered, so too is the relevance of behaviour and psychology to controlling COVID-19. To assess the validity of this retort, let us consider two of the interventions that have been most discussed in recent weeks. One is the wearing of face masks. The other is the use of ‘Test, Trace, Isolate’ (TTI). In other words, find out who is infected, find out who they have been in contact with, isolate those people so they cannot infect others and, in that way, nip the spread in the bud.
The issue around face masks seems very simple. The masks available to the public probably do not prevent a tiny virus getting through and infecting you. But they do stop you breathing, coughing and spluttering the virus over others if you are infected. Overall, it seems a no-brainer: wear masks and reduce the virus spread. Where is the psychology in that?
It is worth starting off by making a small but important distinction. By itself, a mask does not stop anything. It is wearing masks that makes the difference. And wearing masks is a behaviour. Then, just as with the behaviour of staying at home, the question is will people do it or not? Furthermore, the literature on the effectiveness of mask wearing to prevent infection provides rather mixed results. If you wear them properly and dispose of them carefully, they probably have a modestly positive effect (Greenhalgh et al., 2020). But people do not wear them properly. They fit them badly, they lift them to speak, they touch them, they leave them lying on surfaces, and they casually toss them aside. And if they do too much of this, masks may do more harm than good. There are very few high-quality studies of how people actually use masks in everyday settings. But such behavioural investigation is crucial before we can really determine if masks are worthwhile.
And then, there are all the impacts of mask wearing that go beyond the physical impact of the mask. Will they cut us off from others, dehumanise us, further isolate us from other people even when we venture out of our homes? Will they signal danger, increase anxiety, and serve as a further detriment to mental health at a time when people are already scared and anxious not only of getting ill and dying, but also of the economic and political hardship that the pandemic is causing? Will they cause social division and even conflict between those who do and do not wear masks — so that some people accuse others of acting recklessly and foolishly? Conversely, insofar as masks serve to protect others from us rather than us from others, will wearing them create positive social norms? Will masks serve as a public sign that people are acting for the common good and hence strengthen impulses towards kindness and compassion? These questions are just some of the many ways in which the impact of masks on the trajectory of COVID-19 is critically dependent on psychological considerations.

Similar points can be made about ‘Test, Trace, Isolate’. Briefly, the strategy is totally dependent on people’s willingness to be tested, to be tracked, and then to isolate themselves. And hence compliance is as important here as it is with lockdown and with mask wearing. The issue of tracking is particularly problematic. In many countries, people are being asked to download an app onto their phones that will continuously collect data about their proximity to others (or, rather, to others’ phones). Then, if someone tests positive, this information can be used by health agencies to trace the people with whom they have had contact. But will enough people comply to make the system work? Will they be happy with a state agency having such detailed information about their social interactions? In particular, will groups who are more antagonistic to authority willingly submit themselves to this type of ‘Big Brother’ surveillance?
What these examples make clear is that there are a great many psychological issues that shape the impact (for good and for ill) of every measure that governments around the world are contemplating or using to deal with the pandemic. And just as the pandemic itself is unique in our lifetimes, so too we see for the first time a realisation by governments (and by society more widely) that it needs to harness psychology as a key element in strategies to defeat COVID-19. Moreover, and this really is new, governments are seeing psychology not only as relevant to individual-level outcomes (e.g., the effects of the pandemic on mental health) but also as integral to societal level outcomes (e.g., the maintenance of social cohesion or conversely the development of public disorder).
However, it is not enough to understand that we need psychology as a core part of efforts against COVID-19. It is also important to understand what sort of psychology helps or hinders in those efforts.
We need a psychological analysis that recognises people are the solution not the problem
Both within and beyond the academic discipline of psychology, there is a longstanding and influential tradition which views people as mentally frail, beset by biases, and unable to deal with uncertainty, complexity or stress — and therefore prone to unravel completely in a crisis. This kind of psychology holds that when the going gets tough, the people panic (an idea we will examine in more detail in Sections B and D). When the crisis hits, the people become part of the problem. So, they need to be shielded from harsh truths, and shepherded by a paternalistic government who must factor in the frailty of the masses when deciding what forms of disaster management are viable.
We have seen various aspects of this ‘frailty’ tradition in responses to COVID-19. As the dangers posed by the virus began to become clear, the media was full of stories of ‘panic buying’. We were warned that people did not have the willpower to sustain prolonged restrictions and that ‘behavioural fatigue’ would set in. And after lockdown was imposed, the media shifted their attention to so-called ‘covidiots’ who were flouting regulations, flocking to outdoor spaces, and organising indoor parties.
This lack of trust in the psychology of the people had important practical implications (Reicher, 2020). At worst, it was used to undermine medical recommendations as to what measures were needed to control infection. In many countries, the concept of ‘behavioural fatigue’ was notoriously invoked to justify a delay in lockdown. It also encouraged a punitive response towards those who failed to adhere to lockdown regulations. The notion that such non-adherence (e.g., going to the park) was the product of psychological weakness or malevolence led to threats of both individual punishment (imposing fines) and collective punishment (closing down the parks).
There are many problems with such an approach. The first is that it is contradicted by what actually happened. In many ways, the headline story of COVID-19 is not the weakness but the strength of the people. Breaking the rules tends to make better headlines than observing the rules, and so stories of people plundering supermarket shelves for toilet rolls or flouting lockdown have filled the front pages (e.g., see Figure 4 in Chapter 4). Nonetheless, the overall figures show that very few people stockpiled scarce commodities. Equally, the great majority observed restrictions (indeed, far more than authorities in many countries had expected). And it was not easy. One analysis shows that, of the 92% of the UK population supporting lockdown, roughly half (44% vs. 48%) were suffering hardship as a result of the lockdown. It is no hyperbole to say that their behaviour has been heroic.
What is more, when people did violate the lockdown, this had less to do with psychological frailties than with practical difficulties. One particularly telling study showed that the poorest people in Britain were three times more likely than the most affluent to go out to work (Bibby et al., 2020; Smith, 2020). But, crucially, there was no difference in their psychological motivation to stay at home. It was simply that they needed to go to work to put food on the table.
The implication here is that, when attempting to increase adherence, waving a big stick at people generally misses the point. Instead of seeking to enforce lockdown on an unwilling population, the priority must be to enable people to do what they actually want to do. If they leave home from economic necessity, then provide the funding that allows them to stay in. If they leave home to exercise (as they are allowed to do in many countries) and inadvertently find themselves in crowded parks, then make available more green space (such as golf courses and playing fields) so they can keep a safe distance.
It is worth dwelling on this point for a moment, for it illustrates another central theme of this book — the role of social inequalities in this crisis and the impact of this crisis on social inequalities. The following statement was made by an inhabitant of the Paris suburb of Clichy-sous-Bois (a suburb with a high proportion of residents of North African descent), but could be from almost anywhere:
People are trying to respect the lockdown, but what do you do if you’re a family of five or more in a small apartment on the 15th floor? How do you keep children in? How do you feed them when the markets where you buy cheap fruit and vegetables have closed and you can’t afford supermarkets? How can families whose children normally eat in school canteens now make three meals a day?”
This makes the point that poverty has placed significant demands on people which have limited their ability to comply with lockdown regulations (a point we develop further in Section E). Moreover, if these demands led people to venture out, the French state intervened with severe sanctions. In the first sixteen days of lockdown alone the police carried out 5.8 million controls and issued 359,000 fines (FR24 News. 2020). Little surprise that suburbs like Clichy-sous-Bois were the origins of rioting which then spread across France.
This takes us to the second main problem with the ‘psychological frailty’ perspective. It is not just wrong to see people as the problem in a crisis, it is also dangerous. On the one hand it leads policy makers to look to psychology as the basis of problems of adherence and so ignore the real practical problems people face (much like the famous story of the British guns in Singapore pointing out to sea and thereby ignoring the fact that the real threat came from the land). On the other hand — and potentially even more seriously — a punitive approach may actually corrode the public’s motivation to accept measures put in place by the authorities, breed resistance, and even lead to social disorder.
But the most important problem with the ‘psychological frailty’ approach is not the problems it causes, so much as the opportunities that it misses. For it is not just that the public proved very willing to comply with what they were told by the authorities. Rather, the public have played a highly active role in this pandemic. In many countries, they pushed governments into taking action, both to implement policies like lockdown and to provide the packages of support to make adherence possible. Moreover, across the globe, the mutual self-help shown at neighbour, street, community and national levels has been overwhelming. For instance, in the Netherlands, COVID-related volunteering has been at levels not been seen since the North Sea flood of 1953 (van Dijke, 2020). And this is only the tip of the iceberg. In many countries, formal groups have been supplemented by countless individual acts of kindness to erstwhile strangers: putting notes offering help through the door, baking cakes, delivering shopping, and much else besides.
In so many ways, then, the public have not been the problem but a key part of the solution in this pandemic (Levy, 2020). They have not been a source of frailty but of resilience. Indeed, arguably, their response has been the most precious resource available in combatting COVID-19. The role of governments should be to support and enlist this public resilience. As we discuss further in Section B, the ‘frailty’ perspective encourages governments to ignore or even to suppress community solidarity and resilience — an error of tragic proportions. As a counterpoint to this, what we therefore need is a psychological perspective which addresses the roots of such resilience and which can therefore help us understand how it can be developed, nurtured and sustained.
At one level, the solution to this is very simple. It requires recognition that resilience is more than a personal quality located inside particular people. It is also a collective quality that develops between people (Williams et al., 2019). It arises when people come together as a group, when they come to see others as a source of support rather than as competitors who stand in their way (Yzerbyt & Phalet, 2020). However, to reach this simple conclusion, we must sweep away a century of anti-collectivism which regards people coming together in groups as a source of deep anxiety and hostility.
We need to get our heads around the ‘we’ concept
Another consensus that has developed both inside and outside the discipline of psychology, and in much of social science, is that individuals are rational and good, while groups are irrational and bad. Indeed, rationality has generally been understood as the enlightened pursuit of individual self-interest (particularly in economics; but for a critique see Akerlof & Kranton, 2010). From this perspective, becoming part of a group is a process of subversion and loss: as we become part of the mass, we lose our sense of self, we lose our capacity to reason, we shed our moral compass, we lack agency and become like sheep — helplessly following the herd. Fine upstanding citizens morph into a mindless mob. Sensible people become victims of groupthink. Thinkers become zombies. According to this model, if you want optimal outcomes, the best advice you can give people (and society) is to stand alone and apart from the group.
We will critique this analysis further in Sections B and D, but already we can see where this logic takes us in the midst of a pandemic. Audrey Whitlock was one of the leaders of the anti-lockdown protests in North Carolina. The lockdown, she argued, was an act of tyranny from central government, and stood in contradiction to the fundamental freedoms guaranteed to her under the U.S. constitution (Owen, 2020). Audrey became infected with COVID-19, at which point she then argued that the requirement to quarantine herself was a further denial of her rights to go out, to mingle with others, and to join further protests. In this way, her consistent and determined pursuit of her individual rights increased the probability of infection spread and compromised the safety of the community as a whole. As long as Audrey Whitlock and others frame COVID-19 as a ‘me’ thing, this pandemic will be longer, deeper and deadlier.
Fixating on the individual ‘me’ is therefore a way of thinking — and a way of acting — which many have recognised as profoundly limiting in a pandemic. As New York’s governor, Andrew Cuomo, put it:
Yeah it’s your life do whatever you want, but you are now responsible for my life…. We started saying, ‘It’s not about me it’s about we.’ Get your head around the we concept. It’s not all about you. It’s about me too. It’s about we. (Slattery, 2020)
Now, in many ways, we could stop here. For Cuomo’s words are hard to improve upon as a statement of the core theme of this book. COVID-19 is not about me, it is about we. If you respond on the basis of me, then everyone is in trouble. If you respond on the basis of we, then the future is far brighter. To make the point, let us reflect on some examples.
Most people’s sense of personal risk of succumbing to COVID-19 is rather low, particularly amongst younger groups (in March 2020 the WHO estimated that while 3% of people who contract the virus will die, the mortality rate is far higher for older people; Fink, 2020). So, if people were making decisions only in terms of what happens to them personally, many might conclude that it is not worth abiding by lockdown, and adherence rates would be much lower — possibly around 25% (the dark green curve in Figure 1). But most people are not behaving in ‘me’ terms. In fact, one’s sense of personal risk barely affects adherence to lockdown at all. Rather, according to data we have collected from nearly 6,000 respondents across eleven countries, what best predicts adherence is a sense of “we are all in it together and we all need to come out of it together” (Jetten et al., 2020). That is, it is thinking in terms of ‘we’ that leads people to behave in the ways that are necessary to control COVID-19. This raises the issue of how to develop a sense of ‘we-ness’ and, in particular, how leadership can encourage a collective mindset. This is a key issue that we address in Section B.
But thinking in group terms is important not only in determining whether we adhere to lockdown and other such measures. It also determines how well we cope. So while physically isolating ourselves from other people has been necessary in order to limit infections and thereby preserve our physical health, this social isolation also has the potential to compromise both physical and mental health. A large body of work has shown that being part of groups is a powerful prophylactic against such conditions. Feeling part of a group, and having a sense that others are there to support you when you need them, reduces anxiety and stress, and thereby improves not only mental but also physical health (Haslam et al., 2018). The question then arises how can we build such a sense of ‘we-ness’‚ of social connectedness — even when we are distanced from each other? How can we keep people together when they are apart? That is one of the great challenges of this pandemic (which is why we referenced it in the title of the book). We address this question in Section C.
One more example of why ‘we-thinking’ is so important concerns the dynamics of solidarity and citizenship. In a disaster of any size, and certainly one as enveloping as this pandemic, the public sector simply lacks the capacity to deal with everyone’s needs. There are not enough police, care workers or community nurses to look after everyone who needs shopping to be done, medicine to be delivered, or just checking in on to see if they are coping. We have already referred to the flowering of different forms of mutual aid which have emerged to fill the gap. But clearly this flowering is dependent on people thinking in communal rather than personal terms, and therefore being as concerned with the needs of other members of the community as with their own needs. To cite Anna Vickerstaff, one of the founders of the U.K.’s mutual aid national network: “we set this network up because we want to make sure that no one in our communities is being left to face this crisis alone”. These questions of collective action and collective solidarity around COVID-19 — how it develops, how it can be nurtured, why it breaks down, and with what consequences are the focus of Section D.
Yet while we see many examples of groups at their best in a crisis, as we will see in Section E, we equally see many examples of groups at their worst. This is no less true in pandemics. During the Black Death, for instance, over 500 Jewish communities were destroyed across Europe. In one single day, St. Valentine’s day 1349, some 2,000 Jews were burnt to death. In many other cities, including Frankfurt-am-Main and Cologne, the entire Jewish population was destroyed (Cohn, 2007). In the current crisis we are also witnessing outbreaks of collective hatred. In India, for instance, Muslims have been blamed for spreading the disease — so-called ‘coronajihadism’. The novelist Arundhati Roy (2020) has argued that “we are suffering, not just from COVID, but from a crisis of hatred, from a crisis of hunger”. Her words are of relevance to many countries. Indeed, the Head of the United Nations, Antonio Guterres described the pandemic as unleashing “a tsunami of hate and xenophobia, scapegoating and scaremongering” (Hudson, 2020).
This raises two final questions. The first is what determines the passage from a community united in compassion to communities divided by hate? As the question implies, this is not a matter of groups or not groups, but rather of how we draw group boundaries and define group cultures. It is a question of whether the ‘we’ includes all sectors of the community — minorities and majorities alike — or whether our community is divided into a ‘we’ and a ‘they’, and also whether ‘they’ are represented as a threat to our very survival. Are ‘the Jews’ polluting ‘our’ wells? Are ‘the Muslims’ using the infection as a weapon? And where, then, do these constructions of groups and intergroup relations come from?
The second question is how do the faultlines in society — between rich and poor, between ethnic minorities and majorities, between the precarious and the comfortable — affect what happens in the pandemic, and how does the pandemic impact those faultlines? As well as what happens to individuals, a crucial issue concerning COVID-19 is what it will do to our society and to the relations between groups within it. This is a key topic that we address in Section E.
Summing up
By now, hopefully we have persuaded you of three things. First, that the COVID-19 pandemic is as much about psychology as biology, and hence that if we are to deal with the pandemic effectively, it is as important for us to understand how people behave as it is to understand how the virus behaves.
Second, the pandemic is about group psychology in particular. People are predominantly acting as members of a community and for the interests of their community; to the extent that they do so, we are likely to come out from these dark days in better shape. However, we must be particularly vigilant about the ways in which the group is defined. If we slip from ‘we-thinking’ to ‘we-and-they-thinking’ then all of us are in deep trouble.
Third, we urgently need is a framework for understanding how people come to form groups, how they behave in groups, the consequences of being in groups, and the ways in which the boundaries of groups come to be drawn more or less conclusively. The social identity approach will help us to do all of these things. As such, the next chapter of this section will spell out some of its key principles.





























































































