 International Debate
International Debate Ebola: The Human Cost of Neglecting the Social Sciences
Recent figures suggest that the Ebola outbreak in West Africa may be subsiding. The media circus is certainly moving on. When the international community comes to learn from the mismanagement of this episode, how many deaths will be attributed to the neglect of the historic lesson: when confronted with a newly emerging infectious disease, social science knowledge is at least as important as biomedical in saving lives. The first line of defence will almost always be social and behavioural interventions that interrupt the movement of the disease through a population. This involves working with that population, listening to them and learning from them. The people of West Africa have paid a very high price for the gung-ho biomedical colonialism to which they have been subjected.
In a recent issue of Nature, Christopher Whitty, from the UK Department for International Development, and colleagues describe the approach now being piloted by the British government in Sierra Leone. This focuses on the provision of small (10 bed) isolation units: ‘facility planners will need to engage with local populations and be flexible enough to adopt better practices as evidence accumulates. Careful collaborative work with communities, building on what is already known from anthropological studies and field reconnaissance, must guide how facilities are located, designed, staffed and operated to maximize social acceptance.’
The tragedy is that it has taken nearly a year to get to a point where such interventions are being ‘piloted’. Moreover, the first UK hospital to open was an 80 bed unit, managed by an NGO, Save the Children, who are struggling to operate it. This may be a triumph for the army construction team who built it in eight weeks but not for the NGO who could not deliver a trained staff team in more or less the same period. Just 28 patients had been treated in the first three weeks of operation and it is not expected to be running at capacity until January. Whatever the Nature article implies, five other units are being built on the same scale.
Community engagement is critical because it has become clear that traditional contact tracing is not acceptable in a population that is, rightly, suspicious of anyone perceived as agents of states that they have no reason to trust. Even if desirable, the states of West Africa lack the capacity to force contacts into quarantine. Ebola will only be contained by voluntary actions, by people presenting themselves for treatment or segregating themselves from their neighbours. Local isolation units will be accessible and can be staffed to a considerable extent by local people with basic training or who have recovered from infection and have some level of immunity. Relatives and neighbours will also be able to see immediately that many people who go into the units will survive – and those who die will be treated in ways that respect their cultural sensibilities.
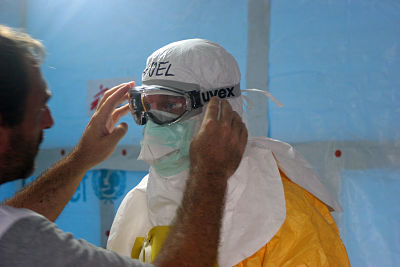
The same spirit needs to be introduced into the burial teams. It is not surprising that people in remote villages react badly to suited and booted Martians coming and seizing the bodies of their kin. This only feeds conspiracy theories about the cause of the outbreak and generates conflict. Where is the effort to understand local traditions in the disposal of the dead? A recent BBC TV News clip featured the reporter asking why they don’t do what we tell them when preparing bodies for burial or practicing voluntary quarantine. It is, however, a basic social science principle: if people don’t do what we ask them to, the problem is ours, not theirs. We have not found the language and way of thinking to connect with the way they are thinking about a problem. I am not an expert on why washing and touching a body is so important to rural people living in West Africa – but I do know that washing bodies is a feature of all the Abrahamic religions and a body soiled by the consequences of Ebola must seem in particular need of care. What effort has gone into devising alternatives consistent with local beliefs? The same clip featured the reporter asking a man who was supposed to be in quarantine why he had gone to the local mosque for midday prayers. He replied that he did not know how to pray on his own, a response that the viewer was invited to dismiss. Should this not be a trigger to involve the leaders of the local mosque to discuss how the flexibility offered by Islam in times of crisis could be invoked to reduce the need for the men to gather together?
These are basic insights that anthropologists, sociologists and other social scientists could have offered from the very beginning and which would have brought transmission rates down with very limited medical input. However, Ebola has been fitted into a colonial narrative where we have to rescue the benighted heathen with our superior technology. An interview on BBC radio with a close friend of one of the Sierra Leonean doctors who had died revealed the frustration clearly felt by many people there with the reluctance of the international agencies and media to reflect the work that was being done by local professionals and volunteers in favour of heroic stories of rescue by Western government agencies and NGOs. The stories about vaccine development are exciting science but this outbreak could be almost completely extinguished before any kind of mass immunization is feasible. Even when it is, vaccinators will face the challenge of gaining acceptance from the people they are seeking to vaccinate. All the virologists in the world will not solve that problem on their own.
Post-outbreak analysis must also consider who is responsible for the weak states and health systems that have failed the peoples of West Africa. Again, social scientists have been pointing for some years at the problems created by the narrow focus of much health and development funding, which has focussed on particular diseases rather than on increasing the capacity of systems.
One of my previous students noted the desperate attempts of a former French colony to spend money that it had been given for the treatment of HIV/AIDS. For a variety of reasons, there were only a handful of cases in the country, while infant mortality from unglamorous diarrhoeal and respiratory diseases was a serious problem. The HIV/AIDS funding could not be diverted to meet real need and actually sucked medical and nursing resources away from the country’s own priorities. The ‘vertical’ approaches favoured by bodies like the Gates Foundation need to be challenged. It is time the World Health Organisation revived the spirit of the Alma-Ata declaration, with its focus on public health and primary care, to become an advocate for the sick rather than a catspaw of the biomedical interests and philanthropic fashions of the First World.
Politicians who ask what the point of the social sciences might be are sometimes right to do so. However, there are also times when the social sciences matter immensely. Newly emerging infectious diseases, epidemics and pandemics are prime examples. On their own, biomedical sciences can achieve only limited impact. In these situations, the application of well-established social science knowledge and expertise will almost certainly save many more lives. We learned this lesson 30 years ago in the early days of HIV/AIDS. It is a tragedy for the widows, widowers and orphans of West Africa that we have failed to remember and institutionalize it.
***
Robert Dingwall is co-editor (with L.M. Hoffman, K. Staniland) of Pandemics and Emerging Infectious Diseases: The Sociological Agenda, Wiley-Blackwell, Oxford, 2013.





























































































